Your day begins as soon as you set foot in your office. Ten patient messages await your attention; an insurance denial on a patient’s MRI beckons from your desk; one of your staff, who manages patient services and scheduling, calls in sick. As you begin responding to patient messages and mentally prepare for the day, you see your first patient pull into the parking lot. Before you know it, the day is over, and you can’t help but wonder how you survived.
At times, practice is anything but what is glamorously portrayed on television. How do you keep up with the day-to-day challenges and curveballs while providing the excellent care your patients deserve? One of the best and simplest things you can do is establish evidence-based protocols. In a clinical setting, a protocol allows you to offer appropriate treatment to patients with little variance and establishes a template that can be individualized based on the patients’ needs. Nutritional protocols should be easily implemented to streamline clinical efficiency and patient treatment, which in turn allows you adapt with ease to the ebb and flow of the not-so-glamorous clinical life.
Let’s talk about nutritional protocols in terms of easy implementation: How can you start making your practice more efficient after you’re done reading this blog post? Three common patient cases that can benefit from nutritional support are symptomatic osteoarthritis, osteoporosis, and tension-type headaches. The number of people affected by these conditions is likely to increase due to the aging population and the obesity epidemic. These conditions have a multifactorial etiology and can be considered the product of an interplay between systemic and local factors. Old age, female gender, overweight and obesity, overuse or disuse, bone density, muscle weakness, and joint laxity all play roles in the development of any one of these issues. Modifying these factors with key nutrients may reduce the risk of these common problems and prevent subsequent pain and disability.
Osteoarthritis is the most common joint disorder in the US. Symptomatic knee osteoarthritis occurs in 10% of men and 13% of women aged 60 years or older.1 An effective protocol should include the following nutrients for minimum trial of three months:2

Many patients may have tried using these nutrients or a combination thereof, and if efficacy was an issue for them in the past, it’s a great opportunity for you to provide some education the wide variance in these products across the market. A fascinating study published in the Journal of American Nutraceutical Association (JANA) conducted by the University of Maryland did an analysis of 32 glucosamine and chondroitin sulfate products across the retail market sector. Of the 32 products tested, 26 of them were found to contain less than 90% of the chondroitin sulfate stated on the label, 17 of those products contained 40% or less and only five of the products tested contained the labeled amount.3 This is important to note because studies show that 800-1200 mg of chondroitin sulfate is necessary for efficacy outcomes. The outcomes will be limited, if any, and patients will get disenchanted with these therapies. Patients need to understand this information and why it’s so important to work with a health care professional who partners with reputable manufacturers in the professional supplement channel and provides products that produce consistent efficacy.
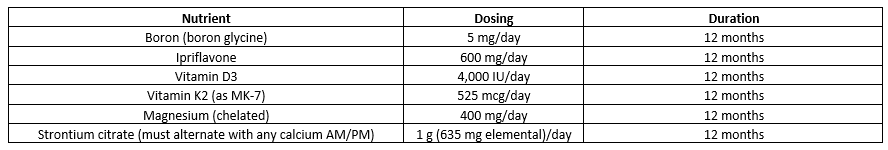
Osteoporosis and low bone mass are currently estimated to be a major public health threat for almost 44 million American women and men aged 50 and older. The 44 million people with either osteoporosis or low bone mass represent 55% of the people aged 50 and older in the US.4 The most commonly prescribed class of medications for osteoporosis are bisphosphonates. While studies show these medications reduce the chance of fracture, they also come with a level of risk. Common side effects may include bone, joint or muscle pain, nausea, difficulty swallowing, heartburn, irritation of the esophagus and gastric ulcers. Severe side effects may even include osteonecrosis of the jaw, femur fracture (long-term use) and impaired kidney function. Thankfully, there are effective alternatives. An effective nutrient protocol should include the following nutrients for 12 months:5
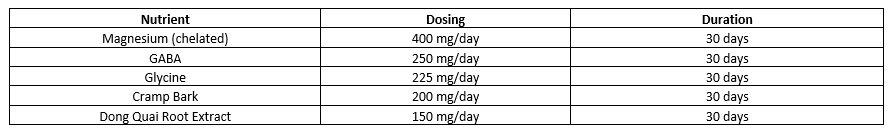
About 30 to 80% of the American adult population suffers from occasional tension-type headaches. Chronic daily tension-type headaches affect approximately 3% of the population; women are twice as likely to suffer from them as men. Most people with episodic tension-type headaches have them no more than once or twice a month, but the headaches can occur more frequently. Many patients with chronic tension-type headaches have usually had the headaches for more than 60 to 90 days. For many headache sufferers, these headaches have a negative effect on their daily activities.6 The following nutrients can be given in combination for headaches triggered by inflammation:7
Nutritional protocols can streamline clinic efficiency and patient treatment. Offer your patients the best, and you will see improved patient outcomes. For more evidence-based nutritional protocols, see our library of In-Practice Guides that focus on topics related to the gastrointestinal tract, immune system, cardiovascular system and stress.
1 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2920533/
2 http://www.pointinstitute.org/wp-content/uploads/2012/10/standard_v_2.3_osteoarthritis.pdf
3 Adebowale, Abimbola & Cox, Donna & Liang, Zhongming & Eddington. Analysis of glucosamine and
chondroitin sulfate content in marketed products and the Caco-2 permeability of chondroitin sulfate raw materials. Journal of the American Nutraceutical Association. 2000.
4 https://www.iofbonehealth.org/facts-statistics
5 http://www.pointinstitute.org/wp-content/uploads/2012/10/standard_v_6.2_osteoporosis.pdf
6
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3444224/
7 http://www.pointinstitute.org/wp-content/uploads/2012/10/standard_v_7.2_Inflammation.pdf

About Adrian den Boer DC, ND
Educated in both the Netherlands and the United States, Dr. Adrian den Boer is a board-certified and licensed Naturopathic and Chiropractic physician. In addition, Dr. den
Boer is fully certified as a functional medicine doctor. Dr. den Boer has treated over 10,000 patients successfully by utilizing multiple resources to manage patient care. Most recently, he joined the Lifestyle Matrix Resource Center as the Clinical
Expert serving the MSK Solutions Pain Recovery Program.





