According the CDC, NIH, and Institute of Medicine, more than 30% of Americans are living with some form of chronic or severe pain.1 To put this in perspective, 116 million Americans live in pain, compared to the 30.3 million who suffer from diabetes, 25.4 million who suffer from cancer, and 14.7 million who suffer from heart disease. More people have chronic pain than suffer from major chronic diseases, and the economic burden and complexity of chronic pain are of epidemic proportions—and growing. Musculoskeletal pain is the number one presenting complaint in clinicians’ offices, and most are ill-equipped to handle it.

Traditionally, pain has been treated with pharmaceutical intervention, but this approach runs a high risk of pill dependency. The CDC reports that 75% of opioid abusers start with a prescription medication, resulting in a devastating 33,091 deaths from unintentional opioid overdoses in 2015. It’s clear we need a better way to address the problem of pain and avoid the trap of pill dependency.

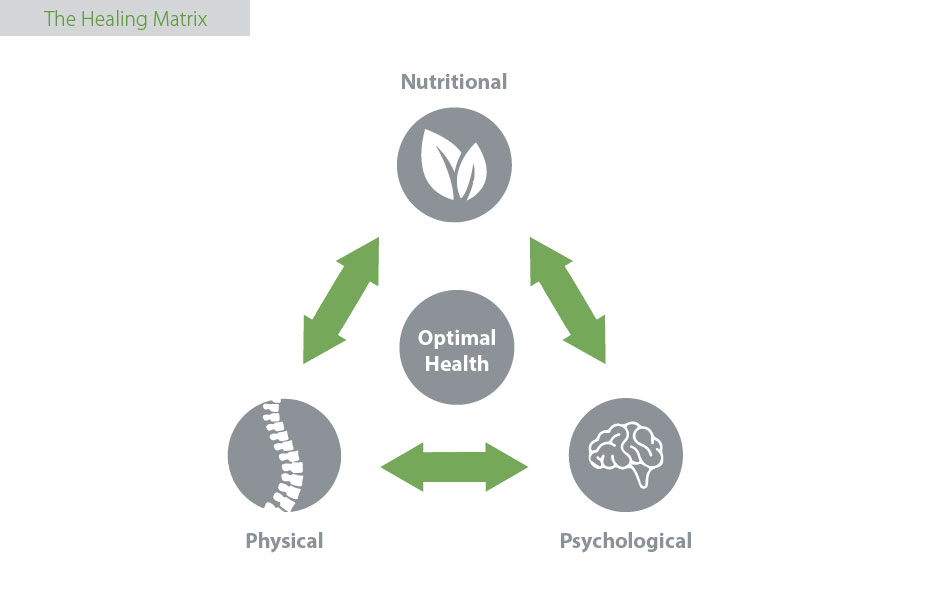
Emerging research on pain management indicates there is more to treating pain than just reducing symptoms. The body is complex and needs a multifaceted approach. Nutritional, physical and psychological aspects of pain and healing should be addressed simultaneously, and make up what we call The Healing Matrix.
Nutritional
Nutrition plays a powerful role in either feeding or resolving inflammation and pain. An anti-inflammatory diet high in vegetables and fruits, supplementation of key nutrients, and rebalancing
bacteria in the gut all ensure the body is reducing harmful waste byproducts that accumulate during inflammation and healing. For example, broccoli contains sulforaphane, a phytochemical with a capability to activate Nrf2 and induce the expression
of a battery of cell-protecting genes, or in other words, changing gene expression to fight inflammation. Turmeric root (curcumin), also displays multiple anti-inflammatory mechanisms that balance the inflammatory response instead of complete inhibition.
Balancing inflammatory response means more complete resolution versus pain management.
Physical
When movement is altered or limited and excess weight is put on the musculoskeletal system, mechanical stress can lead to structural breakdown and limit full healing. Using chiropractic care, physical
therapy, and other manual therapies can lead to increased motion, reduced pain and lowered inflammation. Chiropractic care can increase segmental motion in the spine, allowing more room for nerves to move and inducing a reflex from the dorsal root
ganglion that relieves pain and muscle spasms. Physical therapy and other physical rehabilitation programs can strengthen and restore proper tone to restore previous function. Increased muscular strength can guard against reinjury.
Psychological
The mind influences pain levels, just as pain itself can contribute to psychological distress and depression. The experience of pain can rewire the brain, resulting in harmless stimuli being
perceived as extremely painful. Reducing stress and increasing quality sleep are two ways to quickly decrease pain levels and should be emphasized when treating pain. Focusing on the positive can also help combat chronic pain. According to The Journal
of Positive Psychology, gratitude is related to 23% lower levels of stress hormones, a 10% improvement in sleep quality in patients with chronic pain, and 19% lower depression levels.2
The Healing Matrix goes beyond blocking pain and inflammation pathways in the body and just treating symptoms. Ignoring stress, diet, sleep, and physical activity leaves patients more susceptible to injury. This approach gets to the root causes that drive chronic pain and inflammation mechanisms.

About Adrian den Boer DC, ND
Educated in both the Netherlands and the United States, Dr. Adrian den Boer is a board-certified and licensed Naturopathic and Chiropractic physician. In addition, Dr. den Boer is fully certified as a functional medicine doctor. Dr. den Boer has treated over 10,000 patients successfully by utilizing multiple resources to manage patient care. Most recently, he joined the Lifestyle Matrix Resource Center as the Clinical Expert serving the MSK Solutions Pain Recovery Program.
References
1https://www.cdc.gov/drugoverdose/epidemic/index.html
2http://www.ucdmc.ucdavis.edu/medicalcenter/features/2015-2016/11/20151125_gratitude.html




